In Pursuit of Ikigai:
Standardising Care, Craft,
Rigour & Value in Insurance
Featured: 6th May 2026
⏱️30 seconds Transparency Report Summary
- Health Insurance Cashless approvals got faster: ~6 in 10 approvals cleared within 20 mins; 82.9% within 30 mins.
- Cashless discharge stayed tight: 86.4% closed within 90 mins.
- Health Claims Reimbursements moved quicker: 92% reimbursements were settled within a week.
- Motor Repair go-aheads averaged 15h 44m with 71% approvals completed within 12 hours.
- 75% travel claims were processed through automation.
- Motor proposal processing averaged 30 mins; health proposal processing averaged 6 hrs.
- Post-policy fixes were mostly instant/same-day vs regulator's 7-day benchmark.
- Don't Miss "The Year That Was": Our fast and quirky proof-points from FY26.
- Health claims snapshot: We paid over 2.9 lakh health claims with 97.6% decisioned during the financial year.
- Ombudsman Track Record: Out of 11.16 lakh claims we processed, 339 complaints went to the Ombudsman.
- Systems resilience: Downtime cut ~80% for critical Motor & Health systems; overall reliability at 99.68%.
- Social response sped up: FLR TAT averaged 4m 19s (vs 7.56 mins last year).
- Biggest claims settlements touched ₹2-3 crore in Motor TP; largest health claim reached ₹30 lakh.
- Our Financials: In FY 2025-26, our GWP rose ~10% YoY to ₹11,294 crore, while our PAT rose 28% to ₹544 crore.
“He who has a why to live for can bear with almost any how.”
—Friedrich Nietzsche
In Japan, a question sits behind the idea of Ikigai: why do I wake up every morning? It is not framed in a life-purpose way, but as the everyday pull that gets you up. It blends what you love, what you are good at, what the world needs, and what can sustain you.
As we looked at this, we wondered: if we applied this concept to Digit, what would our Ikigai look like? We realised, for us, it means a path where simplifying insurance becomes a lived reality, and what we do aligns with the four pillars of Ikigai.
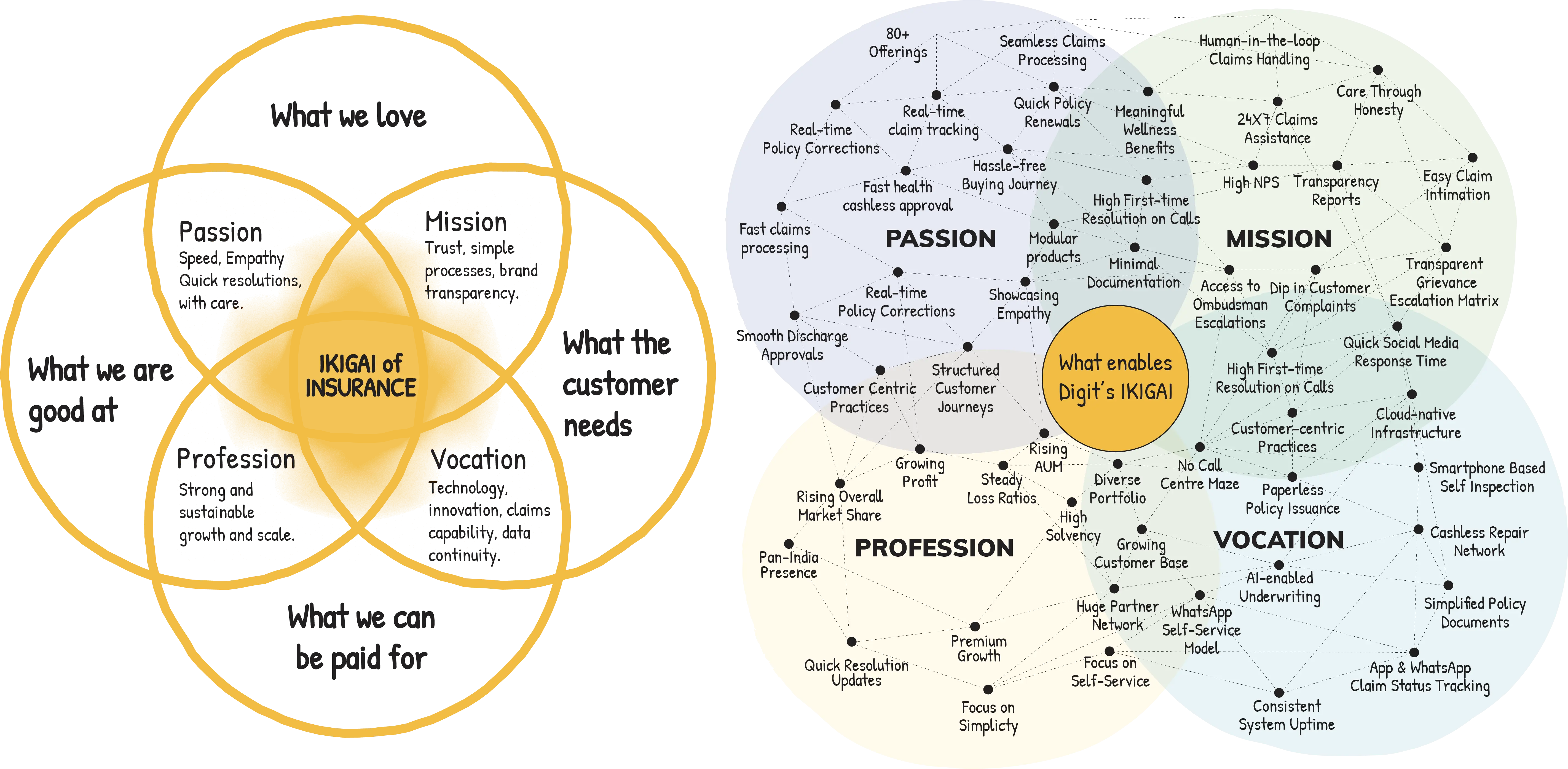
Passion is where what you love meets what you are good at. For us, it shows up as speed with empathy, turning complexity into one-tap solutions and wrapping care in quick resolutions.
Mission sits where what we love meets what our customers need. As insurance often feels complex or opaque, our mission is to rebuild trust by embedding simplification in everything we do and making transparency the default.
Vocation is about being dependable when it matters most, especially in moments of loss. We build systems and technology that scale, so customers get timely resolution, every time.
Profession is about balance: running a healthy business so care stays affordable, systems stay strong, and we keep getting better. Sustainable growth is what keeps our promise real, every day.
In our 14th Transparency Report, we are opening the doors on what drives us every day, the choices we make, and the systems we have built to make our pursuit of Ikigai possible.
PASSION: THE ANATOMY OF SPEED AND EMPATHY
When we thought about what passion means in insurance, one thing became clear: when life goes off track, customers don’t want jargon or fine print. They want reassurance. They want to know that help will come quickly and with genuine care.
That’s why we focus on acting fast, while staying deeply empathetic. Our aim is to make support feel real and present when it matters most. This is made possible by people, processes, and technology working closely together to reduce friction, bring clarity, and keep customers informed at every step. For us, passion is what turns the idea of “making insurance simple” into real, fast, and caring action.
Insider View: Care That Moves Fast
In a hospitalisation journey, three moments typically shape the customer experience most. How quickly a cashless health pre-authorisation is approved, how smoothly discharge is enabled, and how fast reimbursement lands when cashless is not used.
That is why we track TATs closely, to keep the experience calmer, clearer, and more dependable. And averages alone do not tell the full story. That’s why we also transparently share the full TAT distribution, show where most requests land and how even the longer-tail cases behave.
Health Insurance Hospitalisation Claims
Digit pushes cashless requests faster, clears 83% approvals within 30 minutes
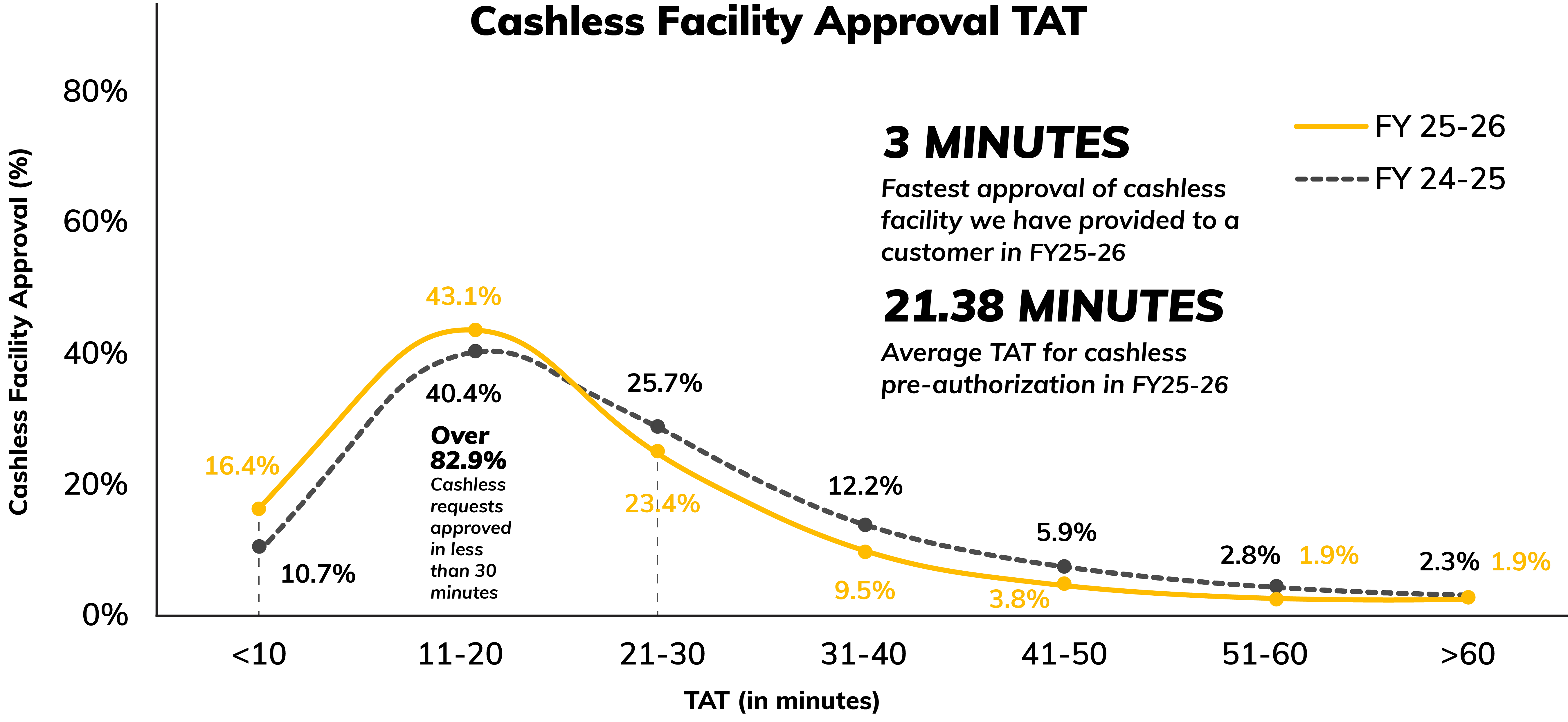
In FY25–26, cashless approvals were noticeably faster compared to last year, with approvals clustering more in the initial minutes. Nearly 6 in 10 requests were cleared within 20 minutes, and 82.9% were approved within 30 minutes. The heavier waits also thinned out, with approvals taking over 30 minutes dropping to 17.1%, and the over 60 minutes bucket easing down to 1.9%. The small tail that remains is typically where extra clarifications or verification are needed to close the loop correctly.
86% cashless discharge approved in under 90 minutes
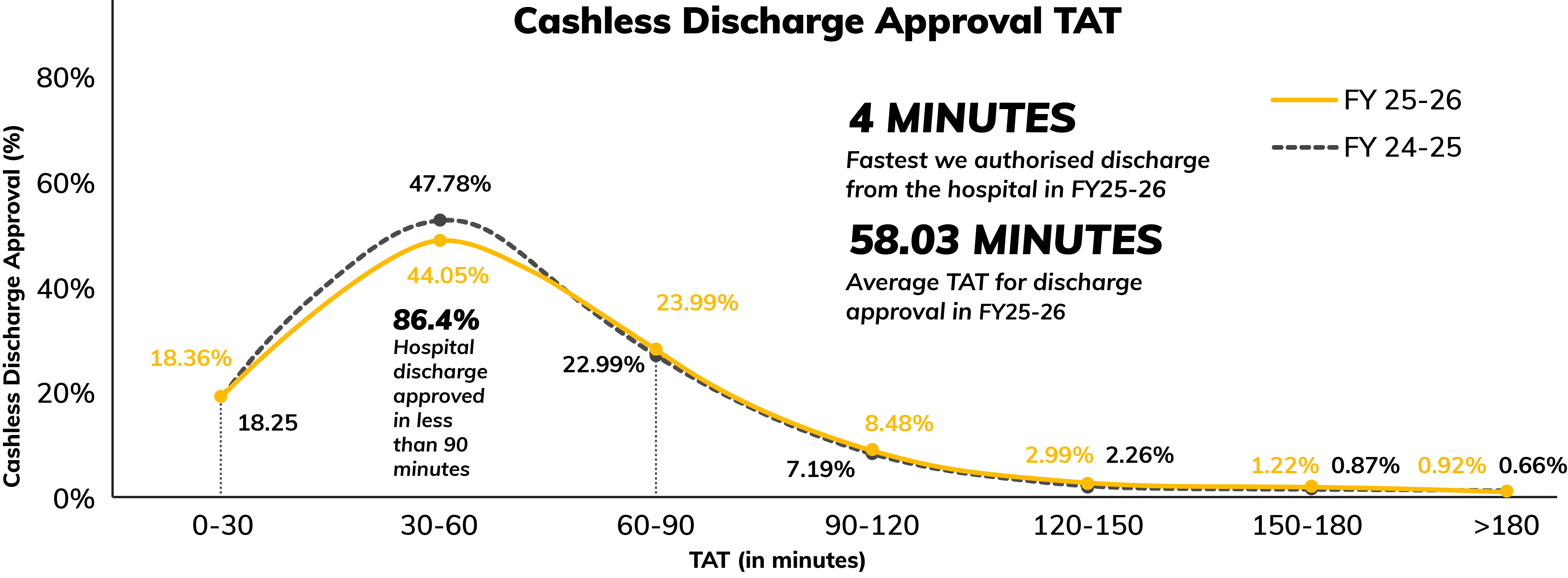
In FY25-26, cashless discharge approvals showed a stronger early push, with a higher share getting closed very quickly. 86.4% of the requests continued to be completed within 90 minutes. The long tail remains tight, with approvals taking over 180 minutes still under 1% at 0.92%. In practice, these longer cases usually reflect complex discharges where additional clarifications are needed to close the loop.
Speeding up health reimbursements: 92% claims settled within a week
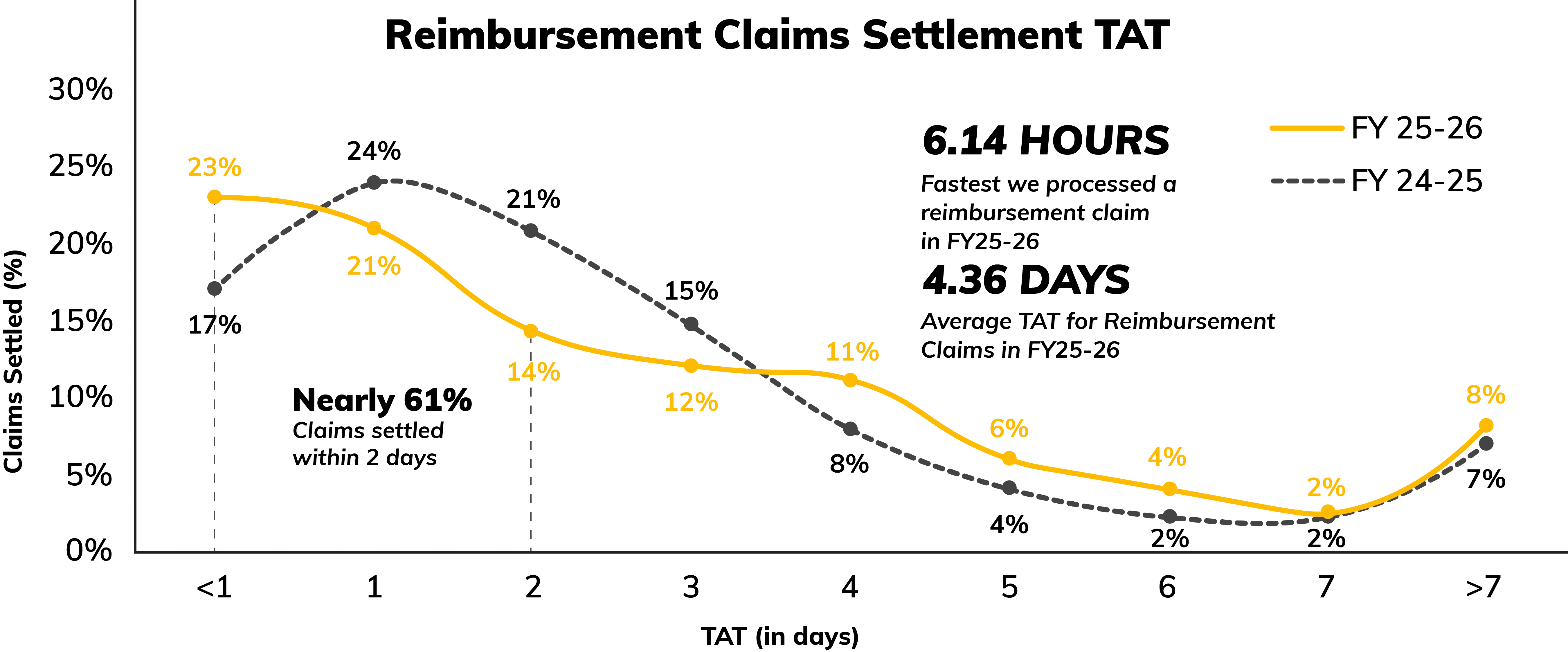
In FY 25-26, reimbursement settlements showed a clear front-end improvement. 23% of claims were settled in under a day, up from 17% in FY 24-25, and 44% were closed within 1 day (including same day), compared to 41% last year. Claims taking 4 to 6 days rose to 21% (from 14%), and the over 7 days bucket edged up to 8% (from 7%), typically where clarifications take longer to complete.
Note: Reimbursement Claims Settlement is the time taken to settle the claim after collating all the necessary claims-related documents.
GETTING YOU BACK FASTER ON THE ROAD
A motor claim is disruption in motion. Customers want the vehicle repaired and life moving again. At network garages, repairs start only after our approval; so, every minute matters. That's why we track this turnaround closely, communicate clearly through the process, and help repairs begin promptly, without unnecessary hold-ups.
Digit speeds up overall vehicle repair go-aheads; 71% approvals completed within 12 hours
In FY 2025-26, our average turnaround time for overall repair approval was 15 hours and 44 minutes. 71% of repair approvals were completed within 12 hours, helping our customers reduce disruption. In FY25-26, private car repair approvals averaged 14 hours 54 minutes, while two-wheeler repair approvals were close behind at an average of 14 hours 37 minutes. Even at the fastest end, approvals were near instant in both segments, at 6 minutes for two-wheelers and 5 minutes for private cars.
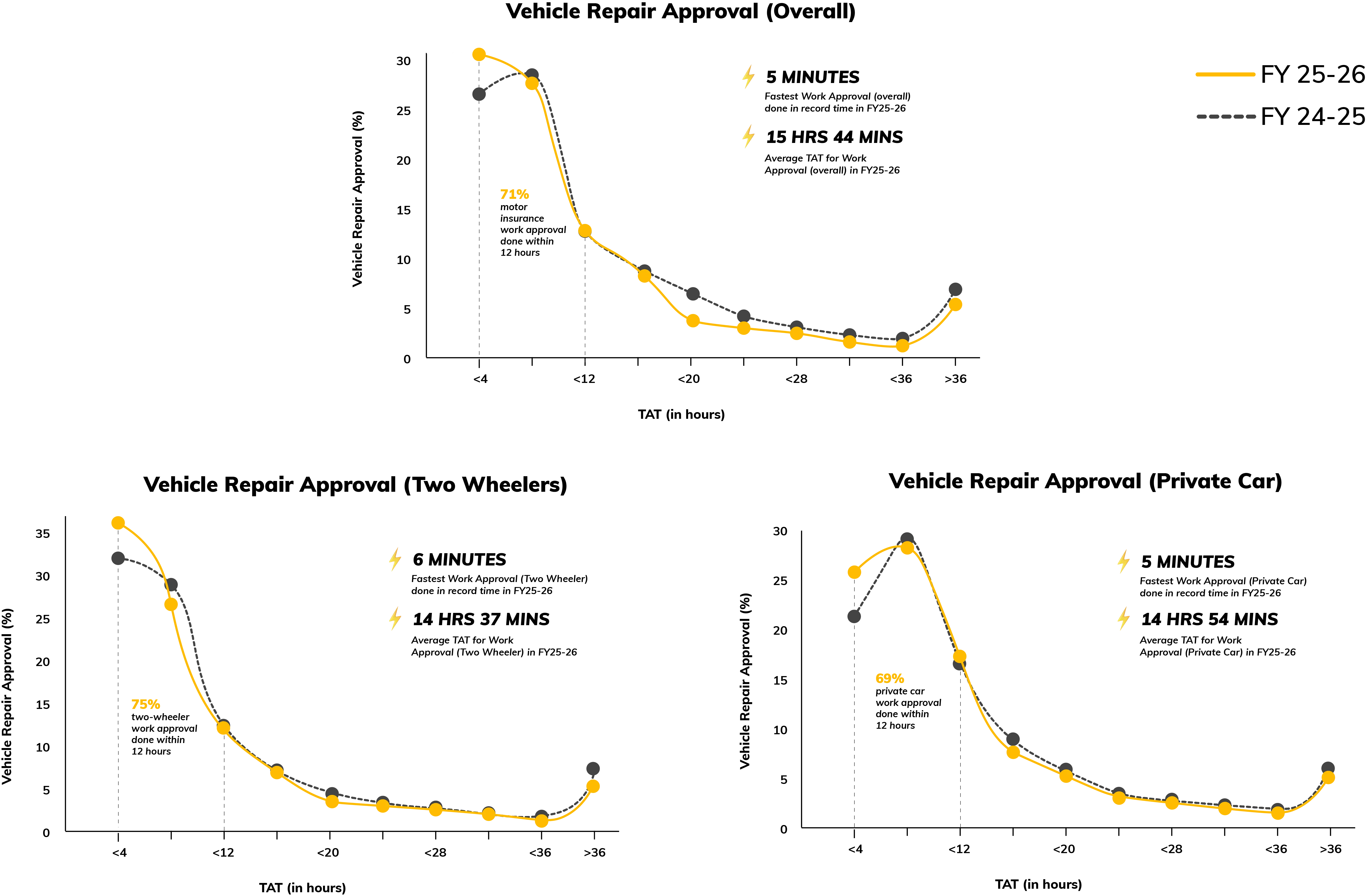
Note: Work Approval TAT refers to the time taken from the First Notice of Loss (FNOL) to issuance of the vehicle repair order. This includes claim intimation by the customer, assessment of claim admissibility, and communication of work approval to the garage for commencement of repairs. While surveys are largely conducted digitally, actual approval timelines may vary based on claim‐specific circumstances.
Digit processes 75% of travel claims via automation
When travel plans go sideways, the last thing you need is paperwork. Our travel insurance is built to move fast, using real-time flight data to automate claims for delays.
In FY 2025-26, 75% of domestic non-medical travel claims were processed through automation. Out of these, 79% were auto-triggered within 15 minutes, leading to faster closure and fewer follow-ups.

Note: Claims auto-triggered indicates claims initiated in system and do not indicate settlement.
THE PULSE OF CARE IN EVERYDAY ACTIONS
Trust isn't just won in the grand gestures; it lives in our attention to even tiny details like how quickly a proposal is processed, a policy document correction is made or how promptly a service request is closed.
While IRDAI sets the minimum standards for these timelines, our obsession with speed means we treat them as a baseline, never the finish line. That is why, for the first time, we are putting some of our service-related TATs out in the open; to show how we perform on the everyday requests that shape customer confidence.
Digit’s Proposal Decisions Sharply Ahead Of Prescribed TATs
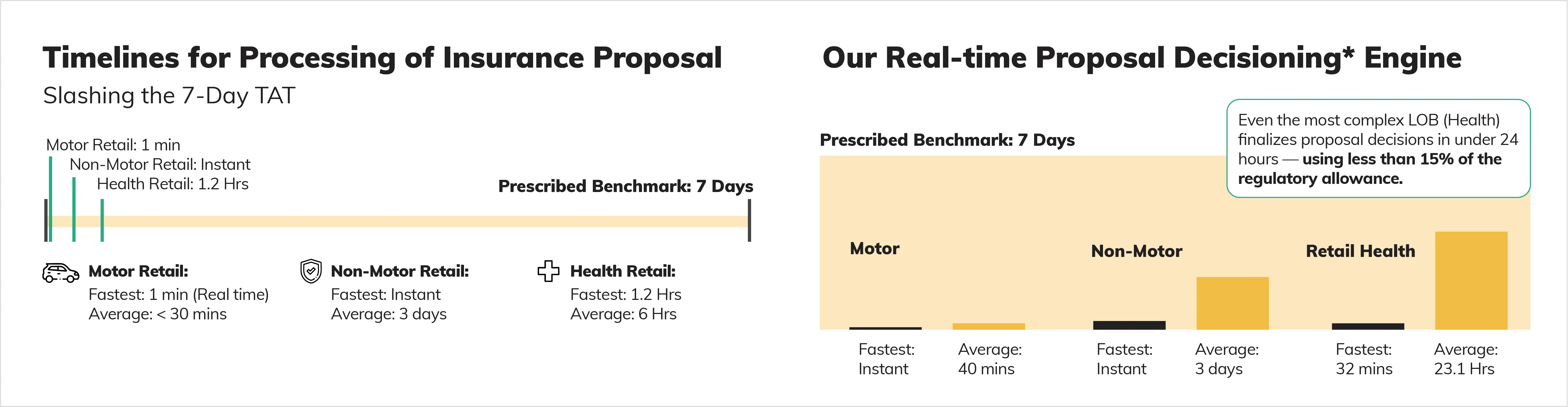
Notes: TATs are based on timelines prescribed in the IRDAI (Protection of Policyholders’ Interests, Operations and Allied Matters of Insurers) Regulations, 2024 and related Master Circulars issued by IRDAI; *TAT of proposal decisioning is calculated from the date of receipt of proposal or from the date of receipt of additional requirement, whichever is later. Data shown not drawn to scale.
Across proposal and policy documentation, our service timelines stay far ahead of the prescribed timelines, turning what can take days into minutes or hours. In FY26, motor retail proposal processing was as fast as 1 minute and averaged under 30 minutes, while proposal decisions were nearly instant and averaged 40 minutes. Non-motor proposal decisions were nearly instant, with average around 3 days for processing and decisioning. Even for health, processing averaged 6 hours and decisioning averaged 23.1 hours, with policy copies typically shared within a few hours, versus the 15-day allowance.
Most post-policy fixes done instantly or same day at Digit; average grievance closure at 52 hours
Post-policy fixes (updation/correction service requests) are meant to feel effortless, and the data shows exactly that. Against an IRDAI benchmark of 7 days, most common requests like change of address, nominations, cancellation & refunds being completed instantly and, on average, within minutes to a couple of hours across motor, non-motor, and health.

Note: TAT of post policy issue service request is calculated from the date of receipt of request for the service specified | *Ref from Master Circular on Protection of Policyholders’ Interests, Operations and Allied Matters of Insurers, 5th Sept 2024.
Grievances should never sit in silence. So, the moment a grievance is raised, acknowledgement goes out immediately through automation, in line with the prescribed mandate. For the actual action and decision communication, the prescribed window is 14 days, but our average closure time is 2 days 4 hours, with the fastest closure recorded at 52:41:04.
OUR CUSTOMER GRIEVANCE RESPONSE

Note: TAT for grievance actioning is calculated from the original date of receipt of complaint
Before we continue with the next Ikigai lens, let's take a look at few bite-sized stories from the year that went by.
DIGIT STORIES: HOW WE COVERED FY2026

*Stacking of dwellings assumption based on Digit’s calculations using average height of homes as 2.75 meters (making combined vertical height of about 466 km); approximate distance between Earth & International Space Station: 400 km. Wrapping of vehicles assumption based on motor policies sold till 31st March 2026. Weighted average of vehicle length assumed at 2.3 meters referenced against the Earth's polar circumference.
A MISSION TO BUILD TRUST THROUGH TRANSPARENCY
Picture this: Riya files a claim and the only question that matters is what happens next. This is the moment our mission is built for. Decisions communicated without ambiguity. Every loop closed, not left hanging. By treating transparency as the default (things we get right and things we don’t), we let customers see all our hits and misses. When you do this, trust follows naturally.
A Deep Dive into Health Claims FY 2025-26
Health claims data only carries weight when the granular numbers behind it reflect real progress. At Digit, we believe you deserve more than just a summary; you deserve a transparent look at how we handle your health claims. Our priority is simple: closing the loop with speed and care. In FY 2025-26, 97.66% of all claims received have already been decisioned, ensuring our customers aren't left in the dark. The remaining 2.34% represent active cases where we are either awaiting essential details from hospitals and policyholders or conducting a final, thorough review.
OUR HEALTH CLAIMS PAYOUT

Note: All data pertains to health LOB excluding PA, Travel; data as on 31 March 2026 | CWP (Closed without payment)
To know what the disposal/decisioned ratio, claims repudiated and CWP ratio mean, read Digit’s Transparency Report 12.
We recognize that for any policyholder, the ultimate measure of an insurer is their consistency in paying versus rejecting claims, so we address that directly. Overall, 7.95% of health claims were repudiated in FY 2025-26. This rate was slightly higher for Retail Health at 7.35%, primarily driven by standard waiting-period conditions—a common feature of retail policies.
Fair Play: Breaking Down Ombudsman Data
For most customers, filing a claim is a stressful experience—one often clouded by the fear of long delays or difficult arguments. When a decision doesn't feel right, the Ombudsman acts as an independent voice to ensure fairness. We don't just track these cases as data points; we look at them as a way to see where we lost a customer's confidence and how we can win it back.
At the start of FY 2025-26, we carried forward 61 cases arising from claims from the previous year that were under the consideration of the Hon'ble Ombudsman. During the year, 339 fresh claim related complaints were registered, bringing the total claim related complaints to 400^.
By the end of the year, 250 of these were resolved, while 150 remained under consideration of the Hon’ble Ombudsman. Of the cases that were resolved, 68 were settled by way of mediation between the customer and us—a reflection of our willingness to engage and resolve concerns. Out of the remaining 182 cases where a formal decision was rendered, 36 were decided in favour of the customer.
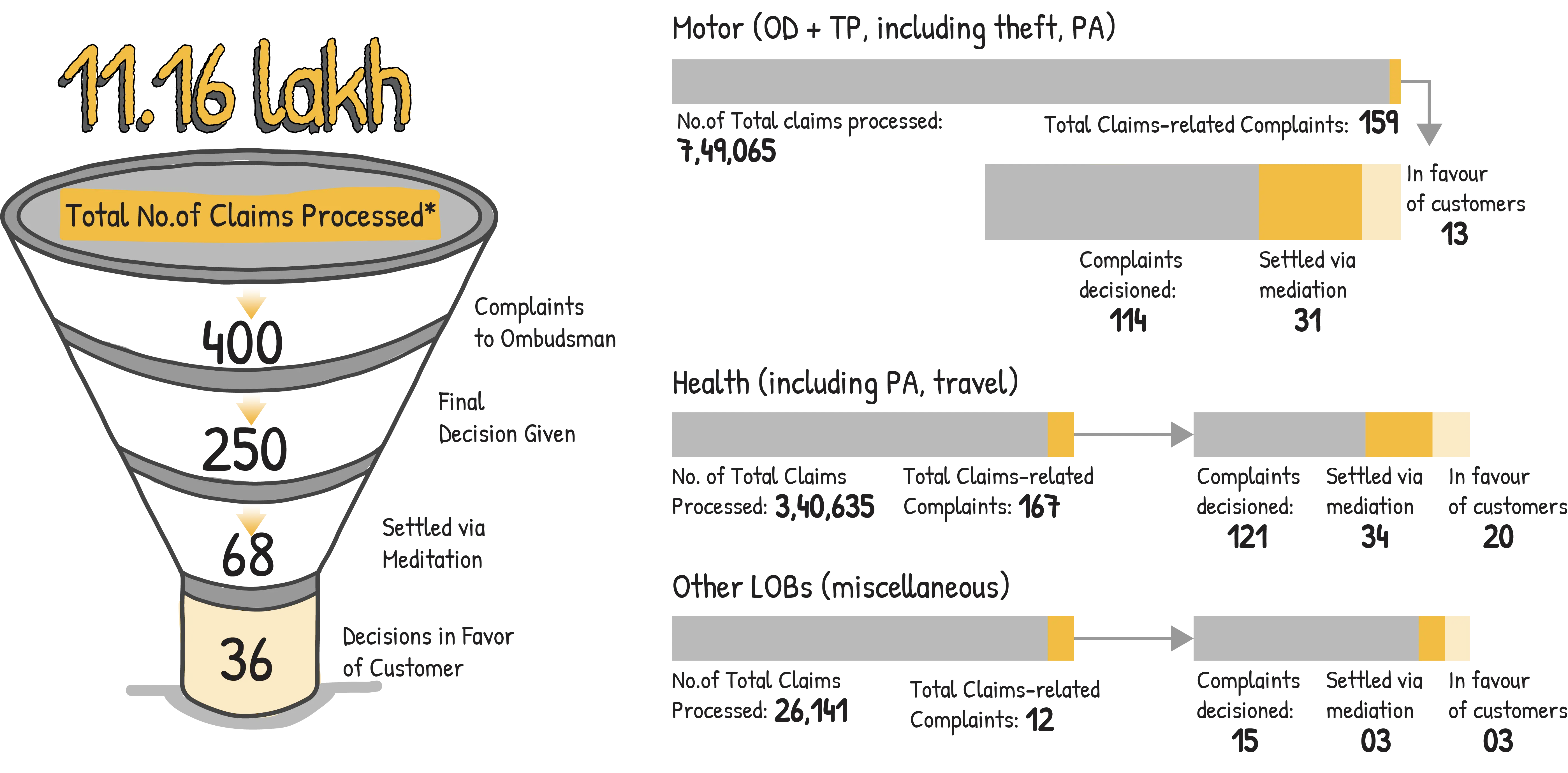
Notes: *Total No. of claims processed in FY25-26: 11,15,841; ^This data pertains to claim related complaints filed with the Hon’ble Insurance Ombudsman (339 new cases in FY 2025-26 + 61 carried forward from FY 2024-25). In FY 2025-26, Company had a total of 13 complaints arising from non-claim i.e. policy related grievances (9 in favour of Company, 0 settled, 1 in favour of customer and 3 remained outstanding). While above data showcases complaints before Hon’ble Ombudsman, customers also have the option to raise their grievance before any judicial/quasi-judicial body including without limitation Consumer forum.
In FY 2025-26, we processed a total of 11.16 lakh claims and out of those, 10.52 lakh claims were paid with an amount involved of ₹5,523 crore. When you contextualise with the data of claims instances escalated to Hon’ble Ombudsman vis-à-vis the number of claims that were processed, we had a claims accuracy of 99.997%. In simpler terms: out of more than a million claims, there were 36 instances where a customer took their case to the Ombudsman and was proven right. Our aim will always be to ensure we pay all the genuine claims.
VOCATION: BLUEPRINT OF RELIABILITY, POWERED BY TECH
Vocation is the high-performance engine where our tech-led strengths meet the scale of the Indian market. Every decision focuses on making coverage easier to grasp and claims easier to resolve, without ever flinching on accuracy or accountability. This is where we do our best work: building simple, digital systems that work quietly in the background, so trust comes from the experience itself and not just from promises.
Staying Online: Systems Downtime Cut by 80%
Insurance does not sleep, and neither do our systems. In FY 25-26, we further strengthened our digital backbone across the website, partner portal, and hospital portal so service stayed dependable when customers needed it most. The impact showed up in the metrics too, with 80% less downtime on critical Motor and Health systems, 99.68% reliability overall, and Health Claims systems availability at 100%. High-priority incidents reduced by 84%, and recurring tech issues dropped by 61%, helping teams focus on meaningful resolutions instead of manual fixes.
FY 25–26 Near Perfection Performance Dashboard
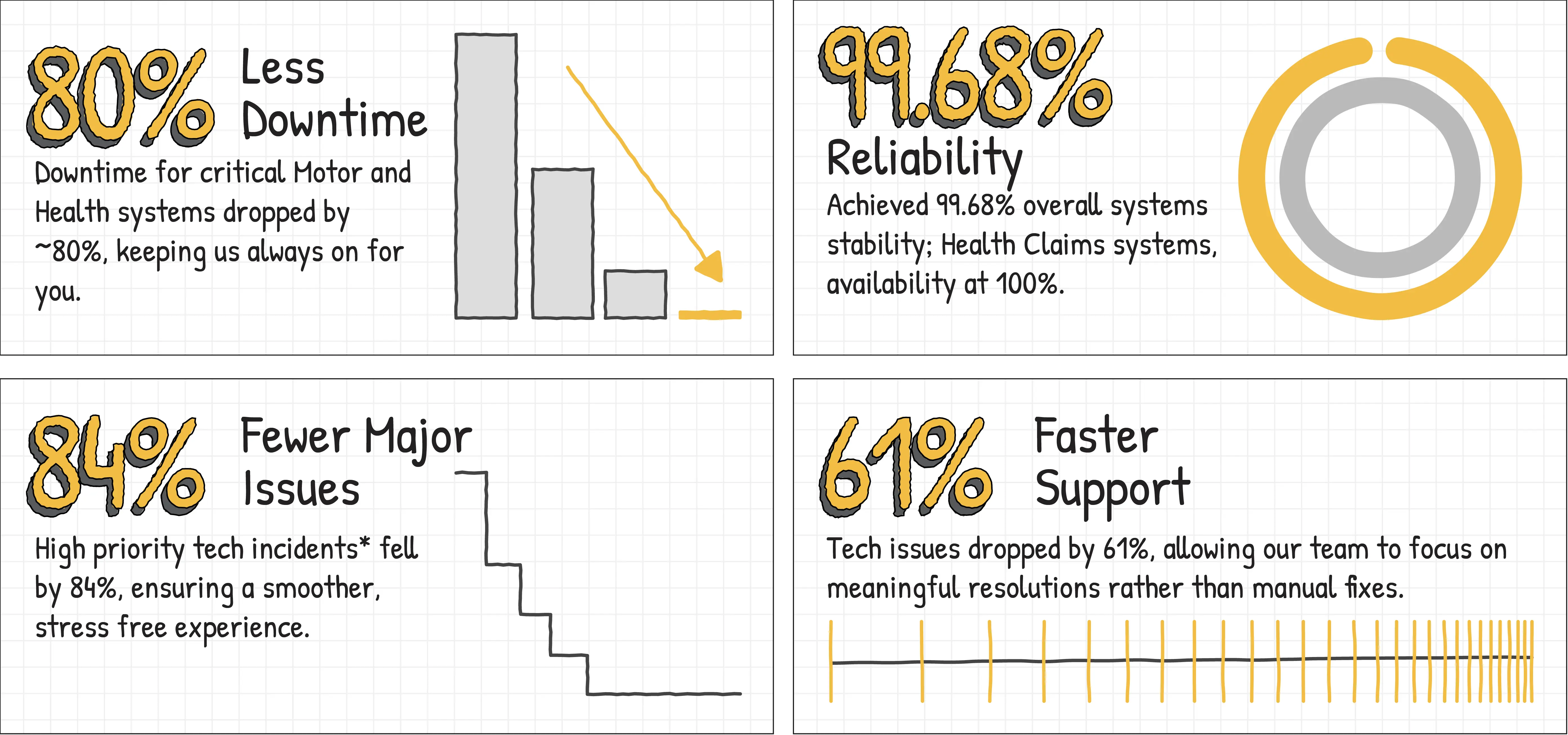
*High‐priority tech incidents are major production incidents impacting customer experience or core business services
How Tech Innovation Makes the Everyday More Reliable
Often, what works well is barely noticed. Behind every ease sit systems built to hold steady as volume grows. Our AI-led tech backbone handles the speed and repetition, while a human-in-the-loop approach ensures we don't trade care for efficiency. Here are few of our innovations making the everyday more reliable.
Agentic AI-Powered Calling: We use autonomous AI calling at scale for reminders, post-policy validations and feedback. Integrated into workflows with monitoring, it keeps outreach timely and purposeful, improving customer connection. We make over 50k outbound calls every month, significantly improving reach and response rates while maintaining strict quality governance.

Automated AI-Driven Motor Claim Validation: We use AI to reconstruct accidents from customer narration and vehicle images, cross-checking impact physics against reported damage. It helps assessors decide claims faster with accuracy. In FY26, this system validated 750 private car claims per day and reduced manual verification by over 125 hours per week.
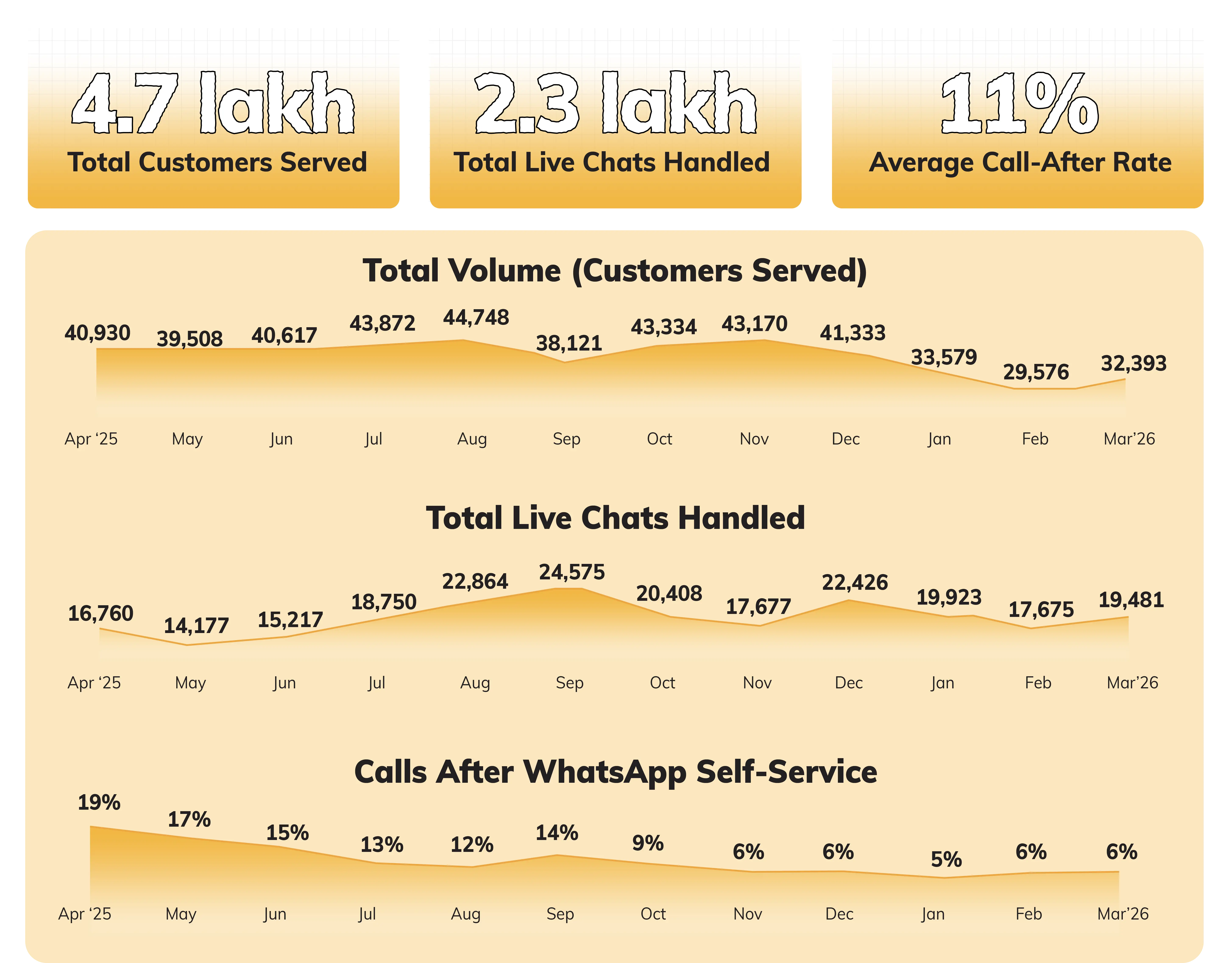
Digit serves 4.7 lakh customers on WhatsApp; cuts follow-up calls sharply to 11%
We've designed our systems to be simple to reach. Over time, more of that work has shifted into places customers already use—like WhatsApp—where renewals, claim updates, and other service requests sit a tap away. The result is that customers have to follow up fewer times.
In FY26, we served 4.7 lakh customers (an average of 1,287 customers per day) and handled 2.3 lakh live chats on WhatsApp. While WhatsApp reduces friction for many needs, not every query ends there. In FY26, the share of customers who used WhatsApp and still called our call centre for next-step clarity dropped sharply to 11%, down from 29% in FY25, showing stronger end-to-end resolution on WhatsApp.
Self‐Service Model That Resolves, Not Repeats
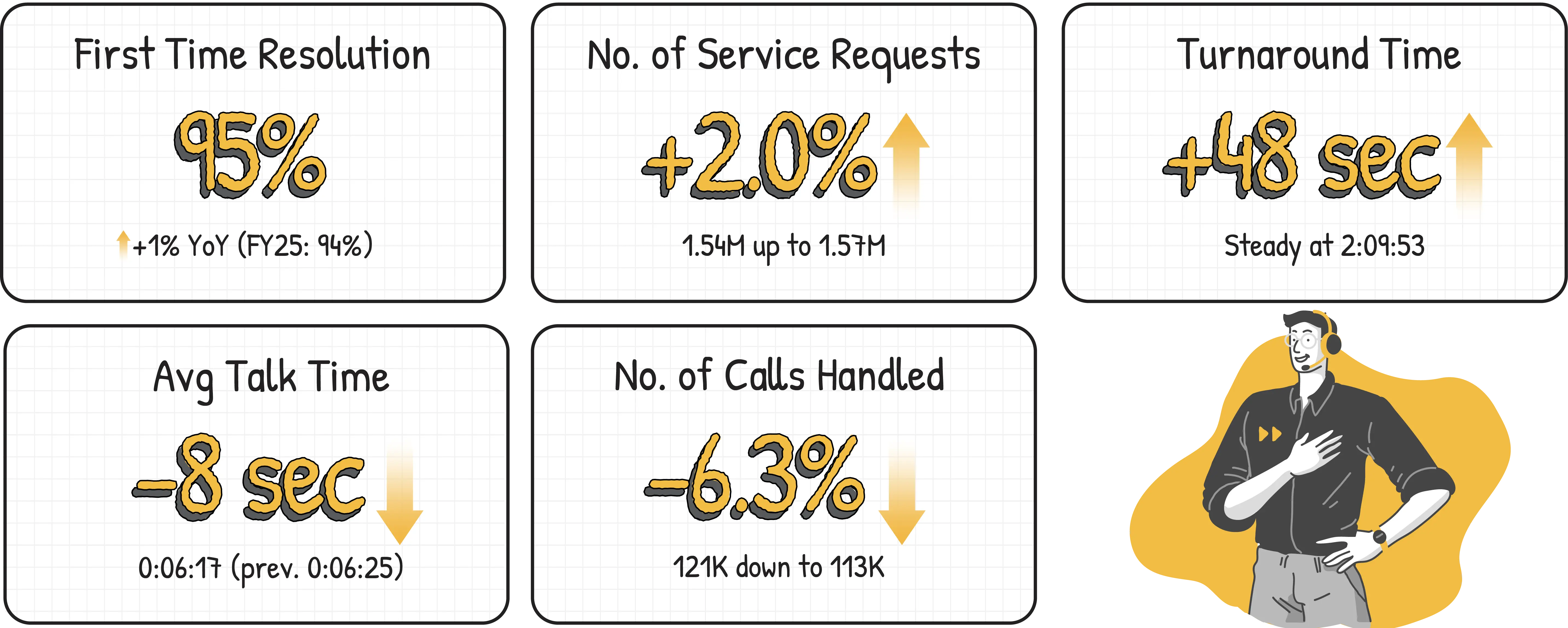
Clarity on First Ring: First-Time Resolution
Improves to 95%
When customers call, the best experience is simple: get the right answer, take the right action, and close it without repeat calls.
In FY26, we handled 113,550 calls compared to 121,253 in FY25, while keeping conversations tighter with a lower average talk time of 0:06:17 versus 0:06:25. Service requests moved from 1,537,898 in FY25 to 1,569,114 in FY26, with TAT staying largely steady at 2:09:53. First Time Resolution (FTR) slightly improved to 95% in FY26, which means customers continued to get closure the first time they reached us.

Social Media: Faster Closures, Clearer Support
Canned replies to customer queries on social media don’t cut it anymore. Customers want to know their issue has been seen, acted on, and closed—not just acknowledged. That’s what we track: the full path from the first message to final resolution. In FY26, our average First Level of Response Turnaround Time (FLR TAT) was just 4 minutes and 19 seconds, an impressive improvement from 7.56 minutes as of last financial year.
In FY26, our average Social Media Closure TAT improved to 1 day and 6 hours, from 1 day and 10 hours in FY25. The only major anomaly was in Jan when our TAT crossed over 50 hours due to few complex cases requiring additional customer inputs, which extended our closure timelines.
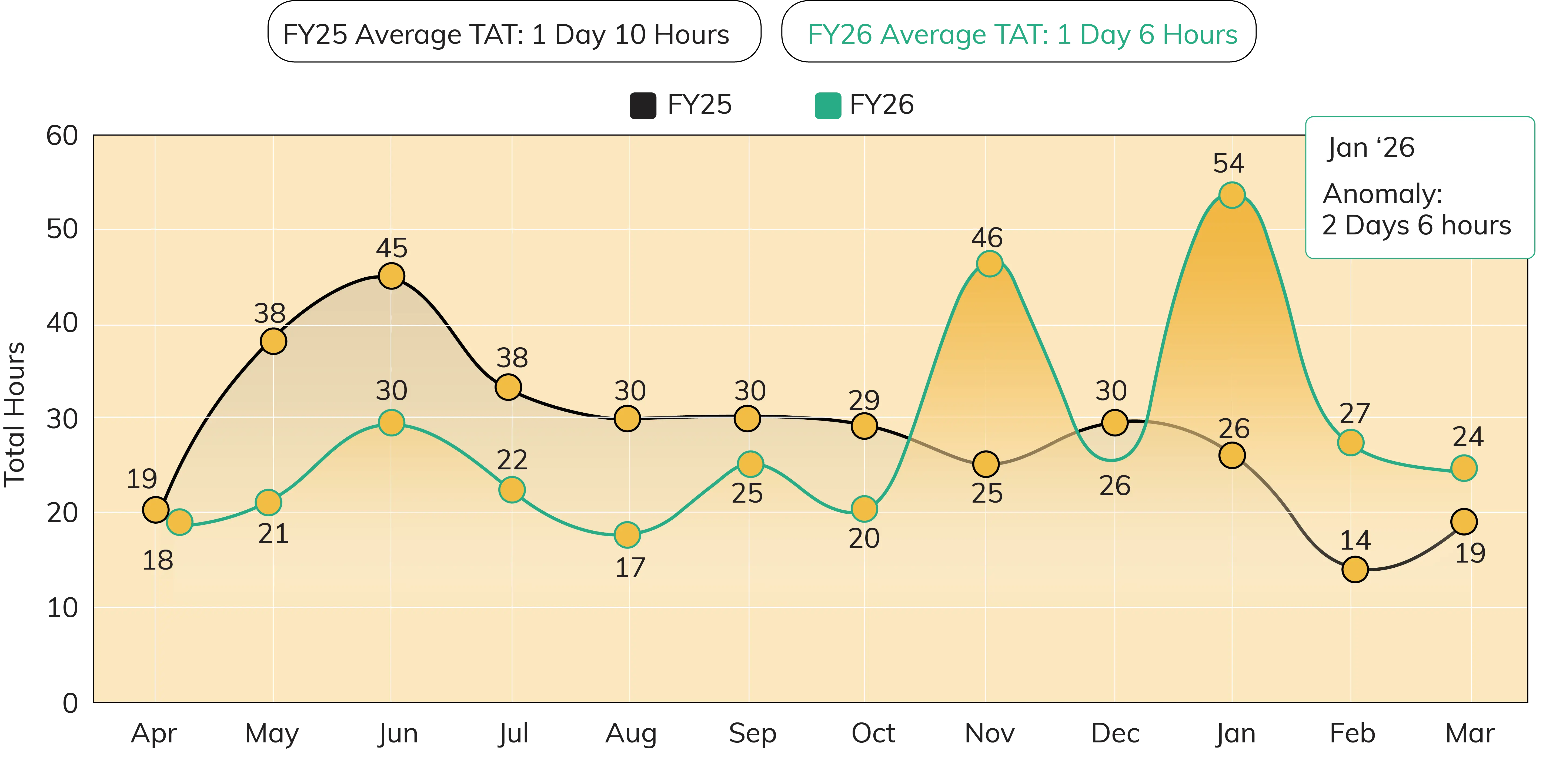
Notes: First Level of Response Turnaround Time (FLR TAT) is the time taken to provide the initial acknowledgment or response to a customer query, comment, or post on social media after it is received. This metric measures the speed of engagement and responsiveness at the very first touchpoint; Social Media Closure TAT is the total time taken to completely resolve a customer query or issue raised on social media platforms. It is measured from the moment the communication is received to the point where the entire resolution loop is closed.
PROFESSION: FOUNDATION THAT SUSTAINS SCALE & STRENGTH
Profession in Ikigai acts as the anchor where the world’s need for security meets the strength of an enduring business. It is the fuel that makes everything else sustainable; the strength that lets an insurer keep promises, keep products affordable, and keep improving experiences.
At Digit, we see this as long-term viability in action. It is the scale that expands access, performance that funds better service, and reach that brings insurance closer to where customers live and work. In essence, this intersection of purpose and profit is what enables our entire ecosystem to endure, allowing our mission to grow stronger and more resilient with time.
Scale With Stability: Our FY2025-26 Snapshot
Growth is not an end in itself. Growth is what gives an insurer the strength to stay dependable, keep products accessible, and keep continuously improving the customer experience year after year. It reflects the ability to invest in better service, build resilience, and honour commitments at scale, even when conditions get tough. You can find our key financials and disclosures here:
https://www.godigit.com/investor-relations

Data for the period FY2025 and FY2026; *Cumulative count of all customers/lives onboarded and includes without limitation persons who have availed insurance benefits under various policies since inception. ^Claims settled since inception | #Asset Under Management numbers are as at March 31, 2026 and as at March 31, 2025
Biggest Claims Settlements Reach ₹2-3 Crore in Motor TP; peak single-day policy issuance crosses 2.2 lakh
A system proves itself when the loss is extraordinary, and when it carries scale. In FY2026, our biggest settlements reached ₹2-3 crore in motor third-party, while the largest health claim touched ₹30 lakh.
Biggest Claims We Settled

CAPTURING OUR GROWTH NUMBERS IN FY 2025–26

*Pincode List in India (Source: India Post )
Behind those payouts sits an engine built for volume. Our 2,602 APIs keep integrations running smoothly across partners and platforms. Our tech ecosystem has helped us issue 2.26 lakh policies on a peak day, process 12,622 claims in a single day, cover group medical policies as large as 2.35 lakh employees and serve 98.5% of India’s pincodes.
A Note on Our Claims Settlement Ratio
We have been regularly publishing our claim settlement ratio (CSR) along with the methodology/formula adopted for its computation. At present, there is an industry level initiative aimed at achieving uniformity in the disclosure and computation of CSR given by insurers. We will resume the publication of our CSR once the final guidance is issued in this regard.
Wellness Benefits in Action: What Customers Use Most
A light cough, a sniffle, a rash; you tend to ignore small signs. You watch, wait, maybe look for a quick answer, hoping it passes. Wellness lives in these moments: quiet, everyday spaces where clarity and early guidance can matter more. Digit's wellness benefits are designed to fit in these spaces.
We have seen an uptick in our wellness offerings over the years. In FY 2025-26, teleconsultations lead at 31%, followed by dental at 18% and diagnostics at 15%, which reflects a clear shift toward early advice and preventive checks. Medicine orders at 10% reinforces the pull of convenience, while the rest is a longer tail across physiotherapy (online & offline), mental therapy, and elder care, signalling comfort with everyday support.
The Wellness Tree
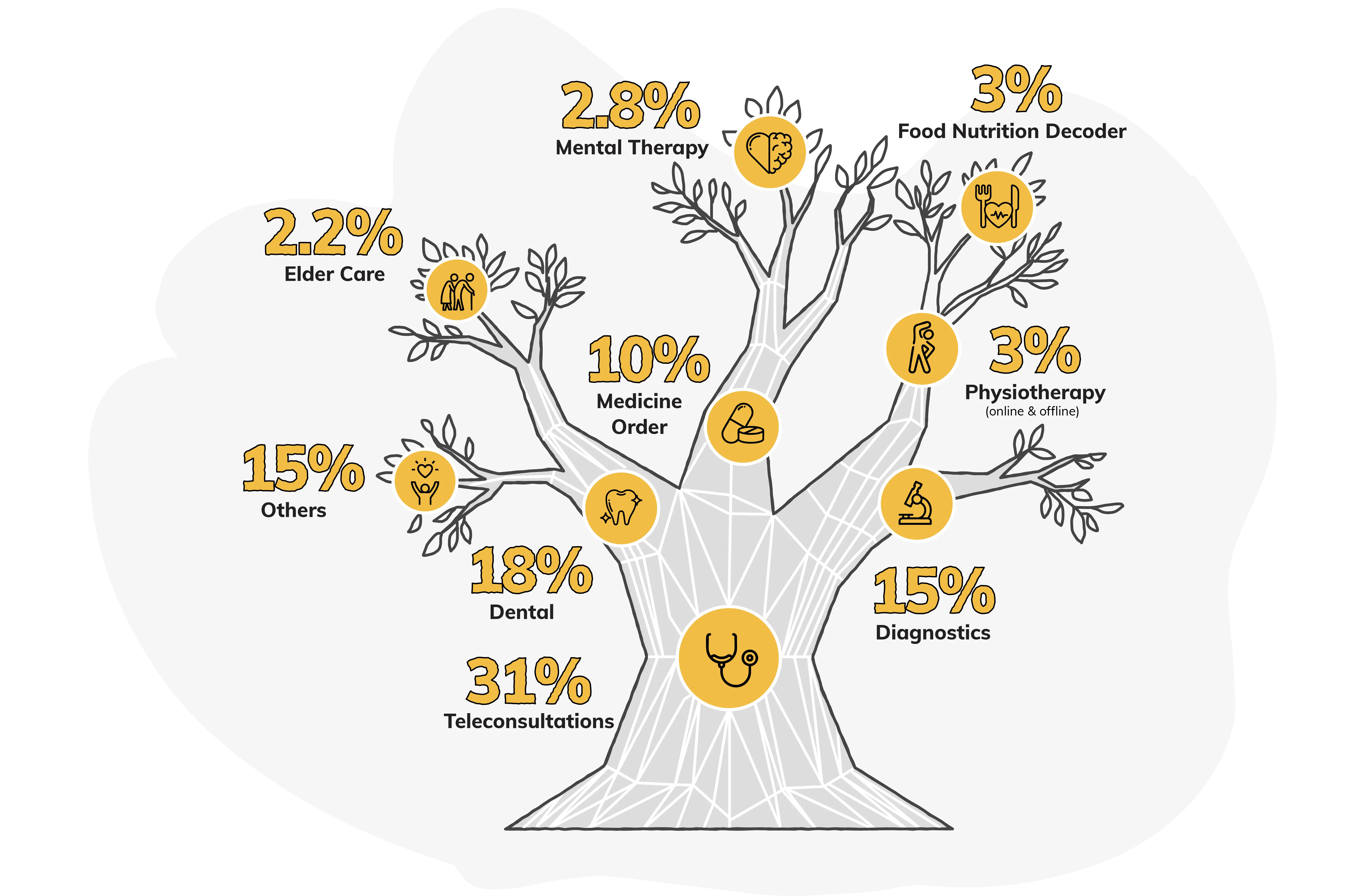
The data reflects customer adoption signals for wellness benefits in FY 2025-26; actual utilisation may vary.
AWARDS & ACCOLADES IN H2FY26

Time to wrap this up. Hope the Transparency Report felt like a breezy 13-minute ride. Write to us at mediarelations@godigit.com and tell us what worked, what did not, and what you want us to unpack next. We will be back with the next drop in October. Until then, take care.



